How Does Baby Fit to Come Out Kf Vagina
When Claire L. found out she was pregnant, she was ecstatic but a petty nervous. Every one of her female relatives on her female parent's side—her grandma, her mom, her aunts, her sister—had needed a cesarean section. Slender hips and big babies were a family trademark.
At virtually twenty weeks, Claire, then 30 and living in Santa Cruz, California, told her obstetrician about her family history. Much to her surprise, the medico waved away her concerns. The takeaway was that practically anyone tin can deliver vaginally. Her relatives' experiences were probably the result of knife-happy, onetime-fashioned doctors. And then Claire went dwelling and did her best non to worry likewise much about information technology.
Similar many commencement-fourth dimension moms, Claire went overdue. A calendar week past her date, an ultrasound indicated that the babe was getting big. She grew nervous again and wondered whether she should be induced. But the doctor had said information technology would be much better to let the baby come when ready. At almost 42 weeks, Claire'due south obstetrician finally said it was time and gave her Pitocin—a drug that jump-starts contractions—assuring her in one case once more that everything would exist fine. It wasn't.
Every bit Claire had expected, information technology was a tight fit, and the baby'south heart rate kept decelerating during contractions. The hospital doctors considered a C-section but pressed ahead with vaginal delivery. When she finally gave nascence to a nine.six-pound daughter afterwards 30 hours of labor and an hour of pushing, the doctors congratulated her: The baby had made it through a rough commitment in perfect wellness.

Claire, not so much. She had three deep vaginal tears, and her labia, her obstetrician told her, were bloated to 50 times the normal size. Shortly after the nativity, she began to bleed profusely—a postpartum hemorrhage caused by the intense stress on her pelvis. She couldn't pee normally for months afterwards, and just sitting acquired excruciating hurting. Forget sex—it wasn't until her daughter was iii months former that she even started to experience better, and she nonetheless wasn't dorsum to normal afterward nine months. "I was told that I'd rest at home for a little bit and then I'd exist fine," Claire told me. "I feel kind of lied to."
Childbirth is, to exist sure, far safer now than it has been for most of human history. In the 18th century, roughly ane in 100 women died in the process—today in the United States, information technology'southward nearly ane in iv,000. Only nonfatal injuries that wreak havoc on a woman'south quality of life remain surprisingly prevalent. Depending on the study, 50 to fourscore percent of women who give nativity experience vehement of the pelvic peel and muscles. For more than than one in x, the tearing is severe enough to damage the anal sphincter muscle, which often leads to the loss of bowel and bladder command. In a 2015 Canadian study, a whopping half of all new mothers were still reporting urinary incontinence a year after the nascence, and more than three-quarters had residual dorsum pain.
The silence of Claire'due south obstetrician on such matters is a problem that infects the entire nascency community. Doctors are required by law to warn women nigh what could happen to their bodies during a cesarean section, from infection to the uterus splitting apart, and pregnant women are routinely informed near genetic weather condition like Downwards's syndrome and nascence defects like spina bifida that could affect the baby. Yet according to more than a dozen physicians and public health experts I interviewed for this story, rare is the obstetrician who has a frank chat with a pregnant adult female about the long-term problems she might face. Even women with the time and money to rigorously gear up for birth seldom hear much nigh how labor and commitment can impairment the pelvic basic and muscles. Childbirth classes gloss over it, as exercise most pop pregnancy books.
First-time mothers are non told that roughly i-third of all women, at some signal in their lives, will develop stress urinary incontinence—a status wherein a cough, a sneeze, or a express joy is likely to cause an "accident." Or that surgery for this condition is three times more common in women who give birth vaginally compared with women who deliver by cesarean section. We hear little, if anything, about the likelihood of pelvic organ prolapse, a horrifying condition in which the uterus or float sags, causing chronic discomfort and oftentimes intense pain during physical activities. Prolapse, which usually shows up in center historic period or later on, happens to 4 pct of women who give birth vaginally versus 2 per centum who have a cesarean.
"Once the infant is built-in healthy, the obstetrician calls it a day. If the mother is damaged, she's told, 'Well, what did you look?'"
All told, co-ordinate to a 2008 report by researchers at the California HMO Kaiser Permanente, about 1 in iii women suffer from a pelvic flooring disorder (a category that includes urinary incontinence, fecal incontinence, and prolapse), and roughly fourscore percent of those women are mothers. Women who deliver vaginally are twice every bit likely to experience these injuries equally women who have a cesarean or who have not given birth. For 1 in x women, the trouble is severe plenty to warrant surgery—that's about double the rate of men who undergo prostate surgery. The costs add upwards: The website Healthcare Bluebook estimates that the typical price for a vaginal hysterectomy, one of the most mutual fixes for uterine prolapse, is about $14,400, including infirmary costs, while a float repair surgery for incontinence runs well-nigh $28,000. Nearly one-third of women who have pelvic-floor surgery volition keep to have at least i more than. According to ane study, nursing habitation admissions resulting from urinary incontinence were costing Americans nearly $half dozen billion a year—and that was a decade ago.
Senior homes aren't the only manufacture cashing in. The US market for developed incontinence products (Depends, etc.) is projected to grow from $1.viii billion in 2015 to $2.7 billion past 2020, and it is expected to catch up to the baby diaper market within a decade. Sleek undergarments advertised by models in their 40s are designed for middle-aged consumers. "We're trying to make the product more normal, and fifty-fifty fun," an executive from industry leader Kimberly-Clark told Bloomberg Businessweek, "with real people in our ads proverb, 'Hey, I accept bladder leakage, and it's no big deal.'" (Kimberly-Clark also recently introduced a tamponlike production for women with urinary stress incontinence to "permit y'all express joy without leaks," one ad promises.)
Yet it is a big deal. Not only are these conditions widespread, debilitating, and expensive—they are also deeply humiliating. Women with prolapse are frequently unable to exercise and "are too embarrassed virtually the burl in their vagina to have sexual practice," says Dr. Victoria Handa, a urogynecologist and the manager of the Section of Gynecology and Obstetrics at the Johns Hopkins Bayview Medical Center. In a 2009 study, Handa found that women with prolapse reported great difficulty reaching orgasm and fifty-fifty getting angry in the get-go place. Many incontinent women are agape to run, leap, or even leave home, lest they have an accident in public. And social isolation begets depression. Information technology doesn't help, Handa says, that in that location is still a culture of silence around pelvic problems, especially prolapse: "No one says, 'I can't go horseback riding with you, Ginny. My uterus is out too far.'"
It's hard to pinpoint the contribution of childbirth to pelvic floor disorders in office considering almost hospitals don't rail what happens to a new female parent after she leaves. Newborns typically get fantabulous follow-up care—they see a pediatrician days later nativity, over again several weeks after, and then every few months for their first twelvemonth. For most new mothers, though, insurance covers merely ane visit with a gynecologist, vi weeks afterward nascence—before some pelvic injuries even become apparent. If a woman complains of pelvic symptoms to her regular doctor, good luck: A 2016 survey found that almost chief care physicians didn't screen for prolapse, and those who did believed it was "rare."
Mothers are more involved in labor and delivery decisions nowadays than they've ever been, and however in some ways they are yet treated as something of an afterthought. Hans Peter Dietz, an Australian urogynecologist who studies maternal childbirth injuries, put it like this: "In one case the baby is built-in healthy, the obstetrician calls it a twenty-four hour period. And if the mother is damaged, she's told, 'Well, what did y'all expect? That's what happens when you take a babe.'"
About childbirth classes teach the aforementioned version of labor: hugely pregnant lady has a twinge or ii, the twinges gradually progress into full-diddled, involuntary contractions, and so, following some amount of groaning and yelling at others, she feels an overwhelming urge to miscarry her baby. Afterward 20 minutes to two hours of intense pushing, a squalling infant emerges. At that place is, of class, enormous variation to this narrative: Poke around and you'll find tales of labors lasting anywhere from a few minutes to 75 days. There are many factors that determine the class of labor, from the delivery technique used to the infant's readiness to exist born. Simply a fundamental factor is the mother's body.
The female person pelvis is a bucket-shaped cage of bone and musculus that sits at the lesser of the abdominal cavity. Attached to the meridian of the bucket are ii wide, winglike bones called ilia, jutting out from either side of the tailbone. The body of the bucket has two pubic basic in front and hip basic on the sides, with the dorsum of the bucket formed past the tailbone. The bucket's base of operations consists of a grouping of muscles chosen the pelvic flooring.
For almost of pregnancy, the uterus sits above the brim while the saucepan body holds the bladder and intestines—those organs will get squished out of the manner when the baby passes through. In the third trimester, a woman's body begins producing hormones that loosen the ligaments between the pelvic bones, widening the summit of the bucket so the baby'southward caput can fit inside. As she goes into labor, the opening to her uterus (the cervix) thins, lengthens, and dilates, allowing the babe to pass into the nascence culvert, the vagina.
The list of ways in which the pelvis and reproductive organs can be damaged during this process is practically endless. Virtually women, every bit mentioned, feel at to the lowest degree some vaginal fierce. Simply in severe cases, the perineum—the area between the vagina and the anus—rips completely open, exposing the vagina to unsafe bacteria and leaving the mother unable to control her bowels. Sometimes, as in Claire's case, the infant is too big to fit hands through the pelvis, and the infant's head or shoulders can break the female parent's basic on the way out. In withal another harrowing scenario, a slice of the placenta remains stuck to the uterine wall after the babe is built-in, causing the woman to hemorrhage. If the pelvic floor muscles stretch besides far during commitment, the uterus may sag into the vagina: prolapse. And fifty-fifty afterwards a woman heals from her immediate injuries, she can experience chronic nerve hurting, muscle spasms, or numbness for months or years. Plenty of women make it through a birth okay, only to suffer from incontinence or prolapse years or decades later, for reasons doctors all the same don't understand.
It'southward tempting to dismiss these less-than-deadly problems every bit inevitable side effects of the miracle of life. Haven't women been pushing giant babies out through their tiny vaginas since time immemorial? Isn't this what nosotros're designed for? Yet many of the obstetricians I spoke to say there's been an uptick in traumatic births. That's mainly considering the mothers are older. From 2000 to 2014, the average age at first birth rose from just under 25 to 26.3, and the number of kickoff-time moms over 35 leaped 23 percentage.
This is significant because the chance of complications increases dramatically with age. In 2014, Norwegian researchers studied roughly 170,000 showtime-time mothers and found that their rate of emergency cesareans—the kind doctors perform when something goes incorrect during labor or delivery—was about 7 percent for mothers in their early 20s only 22 percentage for those older than xl. Even women in their mid-30s have an elevated take chances. In the Usa, the overall rate of cesareans (emergency or planned) is 27 percent for mothers aged 20 to 24, only 41 percentage for those 35 to 39 years old.
Why is this? For one matter, explains Dietz, the Australian urogynecologist, the mechanisms that kick off labor don't seem to work as well in older offset-fourth dimension moms, which can make them more likely to get past due—some other risk factor. Older moms as well tend to accept less effective contractions, which can pb to longer labors and extended pushing—which is strongly linked to pelvic injuries. In 2013, for instance, British researchers plant that a woman'southward odds of severe trauma to the sphincter first out quite pocket-size but grow twoscore percent with each infinitesimal she pushes. And because the pelvic muscles and ligaments are less elastic with age, the babies of older moms are more likely to go stuck coming out.
That'due south non all. Obesity and chronic conditions that grow more than prevalent with age, such as diabetes and hypertension, are likewise risk factors for a difficult delivery. In a 2013 study of ii,235 births, researchers establish that 41 per centum of obese mothers and 57 percentage of morbidly obese mothers—more than ane-third of American women at present autumn into i category or the other—had cesareans, compared with 31 percentage of women of normal weight. From 1998 to 2009, according to a 2012 study published in the journal Obstetrics & Gynecology, the rate of severe labor complications including heart attacks, kidney failure, and aneurysm increased by 75 percent during delivery and 114 percent during postpartum hospital stays. For women pushing 40, all of this comes in addition to the heightened difficulty of getting pregnant and carrying a baby to term in the first place. Afterwards chirapsia those odds, older outset-fourth dimension moms often assume the hardest is behind them—until they meet trouble in the commitment room.
Then the number of women at high gamble for serious labor complications is increasing—and at the same time, and then is the pressure level to have a babe with minimal medical intervention. Public wellness experts hold that America'southward current cesarean charge per unit (virtually 32 percent) is excessive, and that vaginal births are usually preferable for both mothers and babies. Assuming all goes smoothly, mothers who evangelize vaginally have fewer infections and blood clots than women who have cesarean sections, and their postpartum recovery time is typically shorter and less painful. Babies delivered vaginally tend to have stronger lungs than their surgically delivered counterparts. Scientists posit that beneficial bacteria babies pick up in the birth canal protect them against asthma and allergies after.
But it's not simply cesarean sections that accept fallen out of fashion. Amongst highly educated women—who are also more than likely to accept babies later in life—forgoing all labor-easing medication has become a badge of laurels. For this we tin thank the natural childbirth motion, which began more than 50 years ago as a reaction to the overly rigid approach of midcentury obstetricians. Upwards until the belatedly 1940s, some women laboring in hospitals were even given an amnesiac drug called scopolamine that erased their memories of childbirth. This was user-friendly for the (overwhelmingly male person) doctors who presided over these and so-chosen twilight deliveries, but many women establish it traumatic. They woke up sore and disoriented, only to exist sent home to intendance for the helpless new human who had appeared in the bassinet beside them.
During the '70s, feminists decided they no longer wanted to requite birth in a stupor, so they began relearning the ancient art of midwifery and experimenting with having babies at home. In 1971, a midwife named Ina May Gaskin founded a nonhospital birthing center at a rural Tennessee commune chosen The Farm. Gaskin and her young man midwives considered their piece of work an act of protest. "It is our bones belief that the sacrament of birth belongs to the people and that information technology should non exist usurped past a profit-oriented hospital organization," she wrote in her 1975 classic, Spiritual Midwifery.
The sentiment spread and a movement was born. It would be hard to overstate Gaskin'southward influence on today's nascency culture, at least in the privileged enclaves where doulas and mindfulness are in and epidurals and cesareans are decidedly out. Ina May's Guide to Childbirth is now the fifth about popular pregnancy book on Amazon, and information technology's not hard to see why: It makes childbearing sound blissful. In first-person nascency stories from The Farm, women refer to contractions every bit "rushes" and expound upon the "ecstatic" experience of labor. "I could feel my babe move me open, and when the intensity of the rushes increased, I only leaned on a tree," i woman writes. "I became more than angry than I e'er had been in my life!" writes another. "There was no hurting, only the nigh extreme sexual pleasance and consummate openness. It was orgasmic."
Now 76, Gaskin lectures all over the world. She has starred in documentaries and given a widely watched TEDx talk called "Reducing fear of birth in U.South. culture." What to Expect When You lot're Expecting, America's tiptop-selling book on pregnancy and childbirth, adopts Gaskin's ideas, encouraging women to write a detailed nascence plan to present to the commitment squad at the hospital, with instructions on everything from mood lighting in the birthing suite to specific medications and procedures to avoid.
Woe to the modern female parent who seeks to escape the painful pushing. A few years dorsum, tabloids began reporting that some celebrities—Spice Girl Victoria Beckham, supermodel Claudia Schiffer, actress Elizabeth Hurley—were choosing to deliver their babies surgically rather than going through the ordeal of labor. This led to a rash of finger-wagging articles, including a 2004 Time slice ("Also Posh to Push?") that warned of an alarming trend of elective cesareans. These were "not the emergency cesareans that have been performed for hundreds of years to rescue babies from women in medical crisis," it read. "Rather, they had an increasingly popular modern-day variation: planned, scheduled operations for all sorts of less-than-critical reasons." Some women even had the audacity to exist "terrified of labor pains and complicated deliveries or want to avoid the vesture and tear on their bodies."

Noma Bar
Dr. Amy Tuteur, a former obstetrician and vocal critic of the natural childbirth motion, told me Gaskin's philosophy "really achieved a lot when information technology came about, because childbirth was very patriarchal." But at present information technology's gone too far the other way, Tuteur says: Nosotros hear all the great parts well-nigh natural childbirth, merely "there is very fiddling virtually women who end up incontinent or with sexual dysfunction or broken bones, because no i really considers that a big deal."
Part of the trouble, says Lisa Korst, a old obstetrician and public health researcher in Los Angeles who studies trends in infirmary births, is the disconnect betwixt what happens in the delivery room and what happens after a new mother leaves the hospital. Medical codes that specify the severity of complications subsequently birth only don't be. "We lawmaking postpartum hemorrhage so badly," Korst says by way of example. "It's not written down how much you bled. There'southward no code for going to the ICU." And if a woman picks up an infection during commitment that doesn't show up until a few days afterwards she'due south released, "that wouldn't be marked in the hospital record."
At the six-week postpartum appointment, doctors seldom look for pelvic injuries. Gynecologists are trained to make sure that the uterus is returning to its normal size and that any tears are healing well and gratis of infection—not to evaluate the muscles and tissue, says Stephanie Prendergast, a physical therapist and founder of the Los Angeles-based Pelvic Health and Rehabilitation Center. This irks Prendergast because many injuries can be diagnosed with a uncomplicated internal exam. "Information technology takes less than 30 seconds," she says. "You tin palpate for tenderness. Can a woman squeeze or push? If not, she is probably having problems with bowel movements."
All of which is a little ironic, because one thing the natural childbirth movement got right was taking care of postpartum mothers. After a infant is born, traditional midwives stick around. They cheque to brand certain a mother isn't bleeding also much, isn't struggling to apply the bathroom—and they continue checking. Merely later on the half-dozen-week appointment, women who requite birth at hospitals are pretty much on their own.
Consider the case of Lauren Henderberg, a 36-twelvemonth-onetime mom who lives in upstate New York. In March 2008, afterwards ii days of labor—and a delivery in which a forceps was used—Henderberg, then 27, had a baby girl. And though she suffered a deep tear and bled profusely, her md cleared her to get out the hospital after just two days. "I wasn't really offered help or counseled fifty-fifty on how to continue the area clean," she told me. Henderberg spent the adjacent six weeks in acute pain, unable to control her bowels. At her half dozen-week checkup, she was nonetheless securely bruised and swollen, but she was told her symptoms were normal and was sent on her manner.
By July, she was still in pain, bleeding, and having fecal incontinence. Her doctor continued to insist zilch was wrong, but Henderberg'southward symptoms were profoundly disabling. She declined invitations from friends and family, giving vague excuses. "When you lot are sitting there and you have an accident or you smell bad, you don't want to go out," she says. "I didn't want to go somewhere where I didn't know where the nearest bathroom was." She went back to her chore every bit a teacher but eventually quit. What if she had an accident in the classroom? To make matters worse, she began having panic attacks, ordinarily triggered past the sound of cacophonous metal, which brought back memories of the forceps.
"They tell you all nigh how a C-section is serious, it's a surgery. Well, guess what? I ended up with ii surgeries!"
Henderberg began to feel more and more than isolated, but the thought of discussing her symptoms with friends and family unit was mortifying. "I really only thought, 'People don't talk most this,'" she says. Finally, after months of silence, she broke down and confided in her mother, who persuaded her to see a different doc. The new doc said her symptoms were nigh certainly non normal. In the months that followed, Henderberg started physical therapy and was outfitted with an internal medical device that stimulated her pelvic fretfulness with electricity and helped her control her bowels. She also received counseling to deal with psychological trauma from the nascency. Her insurance covered some of the costs, but not all; she spent thousands of dollars on various therapies and adult diapers—an actress burden on elevation of her lost teaching wages.
In 2011, Henderberg began writing about her feel, and what started as a cathartic exercise evolved into a blog. "A lot of my friends hadn't had kids yet," she explains. "I felt like I had to tell them my story. I have my master'southward caste. I read. I consider myself pretty educated. But at that place wasn't fifty-fifty any material out at that place that I could have read."
So what's to be done? Certainly I'm not arguing that hospitals should kickoff slicing open every significant lady who darkens their doorstep. They already tried that, basically, and it didn't work. As cesarean rates soared in the '90s and 2000s, so did maternal deaths. The challenge, instead, is to figure out which women take the highest chance of a vaginal childbirth going south, and—this is important—to tell them about it. Doctors can kickoff by warning older women, overweight women, and those with chronic metabolic conditions. These are difficult conversations. "It's politically incorrect to say something well-nigh how waiting till later in life to have your first baby will increment your risk of problems during commitment," urogynecologist Dietz told me. "That's a piece of news that no one wants to hear."
Invariably, the doctors I talked to mentioned that at that place are probably many other risk factors we don't know well-nigh yet, merely they noted that funding to research pelvic injuries is hard to come by—proposals to help former ladies not leak pee don't exactly rake in the grant money. That seems shortsighted, given all the cash to be saved on unnecessary surgeries and premature nursing domicile admissions.
A few doctors—such as Dietz and University of Michigan urogynecologist John DeLancey—are yet studying the toll of pelvic injuries on women. "If I were in their place," DeLancey told me, "I would expect the aforementioned kind of treatment as a guy who tears his ACL or has prostate cancer."
Ten years ago, DeLancey'due south squad began trying to figure out how to prevent some of these harms in the first identify. Using state-of-the-art MRI techniques, the researchers identified 1 injury in particular that dramatically increases a woman's odds of problems later on. At the base of the pelvis, there'southward a small muscle called the levator ani that gets completely torn off the os in most 15 percent of vaginal births. It takes training to find the injury immediately later birth—few doctors know how to exercise so—and later on half-dozen months or so, information technology becomes almost impossible to spot. So the vast bulk of women to whom this happens won't know until years subsequently, when they become incontinent or have a prolapse.
DeLancey and Dietz, working separately, plant that certain women are much more likely than others to experience a levator ani tear. Pushing for two and a one-half hours or more than is one take chances cistron, as are certain body types. Delivery with forceps is the biggest risk factor of all. DeLancey also co-authored a modest 2015 study in which 29 percent of postpartum women at risk for levator ani tears were found to have fractures from childbirth.
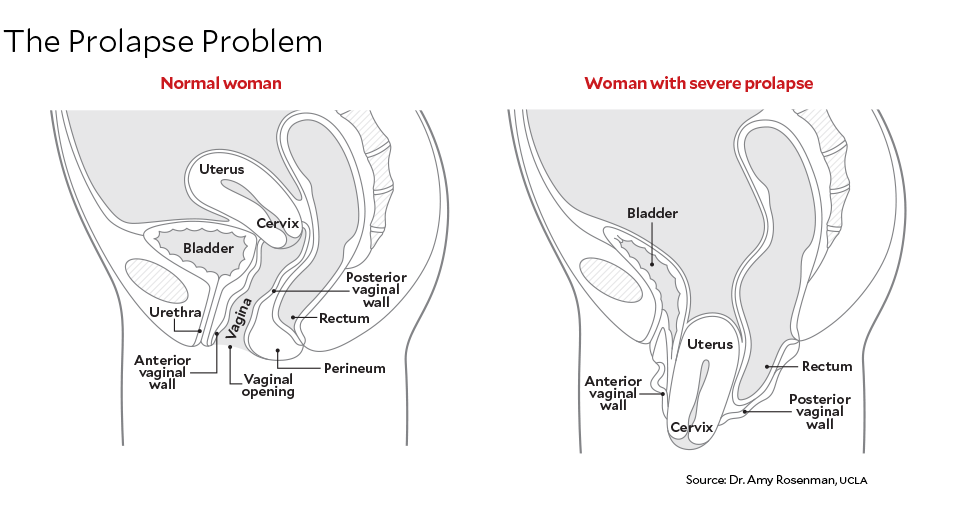
DeLancey introduced me to one of his patients, a 59-year-quondam mother of two I'll phone call Carol. In 1992, after a hard labor—in which the blood vessels in her eyes burst and the baby got stuck in the nativity canal—Ballad gave nascency to a daughter at the University of Michigan Medical Center, domicile to one of the nation's height hospitals. Her uterus and bladder prolapsed and stayed that way for about a decade, through the birth of her second kid—2 surgeries were required to fix the situation. "It affected everything," Carol told me. "I couldn't do whatsoever kind of exercise. It's like having a tampon sticking halfway out all the time. Y'all go really sore."
With further inquiry, DeLancey says, doctors may be able to better predict a adult female's risk for levator ani tears and other pelvic injuries, and mayhap assist women like Ballad avoid them. In some cases, that might hateful a planned cesarean section, but there may be less drastic solutions. Prendergast, the pelvic concrete therapist, points to studies showing that some women with mild injuries can heal completely if they begin a program of elementary exercises correct subsequently giving birth. In French republic, it's common for new mothers to take "perineal reeducation" therapy, like to what Henderberg went through, in which a physical therapist leads the woman through exercises with the aid of an intravaginal electric device. That may sound torturous, just the technique has been shown to dramatically curb incontinence. (Kegel exercises, recommended by childbirth books and classes to strengthen a woman's pelvic muscles, exercise not appear to assist. "Information technology'south what everyone would like to believe," DeLancey told me, "simply I don't remember at that place's any evidence to support it.")
Simple measures taken during birth can also assistance women avert injury. Proponents of natural childbirth frown on the use of epidurals—which deadens sensation in a woman's lower body past means of medication injected into the spinal cord. Just a 2010 study in the British Journal of Obstetrics and Gynecology establish that women who had an epidural were less likely to damage their pelvic muscles than those who delivered without. (Medical testify does non support the merits by some natural childbirth advocates that epidurals interfere with breastfeeding.)
Using labor-inducing drugs such as Pitocin can sometimes lead to a more than traumatic delivery, but induction under limited circumstances may help reduce pelvic injuries. If a baby is unusually large at full term, for example, information technology is often better to induce than wait for labor to commence naturally a week or two later, when a still-larger baby might break his female parent's bones on the exit.
These things are worth considering, even for women put off by the idea of modern medicine crashing their birth-day party, because forging ahead with a difficult labor may really mean more than medical intervention in the long run. DeLancey has performed thousands of surgeries to prepare childbirth injuries. The health care system could prevent a bang-up bargain of suffering, he says, simply by educating the women at loftier risk for pelvic complications.
So at that place'southward this: Telling significant women the truth about their bodies just seems similar the correct affair to do. At the very least, it behooves us to ditch the magical thinking and end pretending that natural childbirth is an amulet that protects women from harm. That goes for the entire nascency community: the books, the midwives and doulas, the Lamaze classes, and near of all, the doctors. Because, quite simply, it'due south an issue of control. If you don't truly know what to expect when you lot're having a babe, and then yous're more probable to shut up and let the physician make the decisions. And so all of a sudden we're back to the 1940s, putting women through hell and giving them a pill to make them forget information technology ever happened.
Carol told me her mind often returns to those agonizing hours on the commitment table. "No one ever said, 'You lot're pushing for too long,'" she says. "They tell you all about how a C-section is serious, it's a surgery. Well, guess what? I ended up with 2 surgeries! I'm ever thinking, 'This would have been different if I had merely known.'"
Source: https://www.motherjones.com/politics/2017/01/childbirth-injuries-prolapse-cesarean-section-natural-childbirth/
0 Response to "How Does Baby Fit to Come Out Kf Vagina"
Post a Comment